Elder abuse is a serious problem that is surprisingly common in the United States that affects the lives of millions of elderly individuals.
According to the CDC, from 2002 to 2016:
- Over 643,000 elders were treated for assault in emergency rooms
- Over 19,000 seniors died as a result of abuse
- 1 in 10 people over 60 living at home were victims of some type of elder abuse
- Elder abuse is presumed to be significantly under-reported.
Elder abuse can result in physical injuries and medical emergencies, but it often does not. However, it can leave a lasting emotional scar even when there are no obvious physical signs.
It is important to be alert and know what to look for to protect all seniors from abuse, neglect and mistreatment in its various forms.
What is Elder Abuse and Why Does it Happen?
Elder abuse is defined as non-accidental action, or failure to take necessary action, that results in real or potential harm to an elder. An elder is considered any person over 60 years old.
There are seven distinct types of elder abuse, which include physical, emotional and sexual abuse, financial exploitation, and neglect.
Elder abuse is often committed by someone that an elder knows and trusts. It can happen when well meaning people are overworked and overwhelmed. It can also occur when a predatory person takes advantage of an elder’s vulnerability.

Factors that Put a Senior at Higher Risk for Elder Abuse
There are certain factors that increase an elder’s risk of becoming a victim of abuse. These don’t always lead to abuse, but they do tend to make it more likely.
Poor Health of the Elder
- Poor physical health
- Poor memory or dementia
- Poor mental health or diagnosis of mental illness
- Tendencies toward challenging behavior (such as resistance to assistance, aggression or mood swings)
Preparedness, State, and Wellbeing of the Caregiver
- Poor training or understanding of the elder’s conditions, needs or how to perform necessary care
- Poor health of the caregiver
- Hesitance to accept help
- Poor coping skills
- Alcohol or drug misuse
- Poor self-care habits
- Difficulty sleeping
Relationship Challenges
- Family history of abuse
- Past or current volatile emotions, behavior or relationships
Living Arrangements
- Elder is living with an unprepared caregiver
- Isolated living situation
- Poor social support
- Few assistive services (such as home care, hospice, counseling, or therapy)
Financial Challenges
- Elder or caregiver are financially dependent on the other
- Limited funds
Risks Unique to Institutions
- Poor staff training
- Chronic staffing problems or overworked staff
- Staff burnout
- Stressful working conditions
- Low standards of care
- Poor administrative oversight
- Physical environment is unclean, unkempt, uncomfortable or in disrepair
The Seven Types of Elder Abuse
There are seven different forms of elder abuse.
1. Elder Physical Abuse
Physical abuse occurs when a person purposely uses physical force that may cause pain, injury or impairment to an elder. Among other things, physical abuse can include hitting, pinching or pushing a senior.
Physical abuse can also include confining or restraining the elder, such as locking them in a room or tying them to a chair to prevent a fall. Even if these are done “for their own good” or safety, under most circumstances these actions violate their rights and are considered abuse.
Physical abuse can result in bruises, cuts, sprains, fractures or other physical injuries. It can also terrify and emotionally traumatize the senior.
2. Elder Sexual Abuse
Sexual abuse includes non-consensual sexual contact with an elder. It can also include forcing an elder to undress or watch sexually explicit images or activity.
There are a wide array of activities that are considered sexual abuse:
- A paid caregiver raping or molesting an elder
- A spouse forcing unwanted intercourse or sexual contact
- A person with dementia inappropriately touching an elder who does not want it or who cannot legally consent to it.
- Forcing an elderly to watch pornography or view graphic images
It is sometimes unclear exactly when someone with dementia, or other health condition affecting mental capacity, is able to consent to sexual activity. Laws vary in different locations. In some cases, mental health experts must determine whether an individual has the capacity to consent.
3. Elder Emotional Abuse
Emotional abuse, sometimes also referred to as psychological abuse, includes emotionally distressing activity such as yelling, threatening, intimidating, ignoring or using hurtful words.
Emotional abuse can also include isolating the elder from their friends or family members.

4. Senior Financial Abuse or Exploitation
Financial abuse includes all kinds of misuse of an elder’s money or property. There is a wide array of activities considered financial abuse, including:
- Theft
- Scams (specifically, scams targeting senior citizens)
- Fraud
- Identity theft
- Withdrawing money from a bank account, writing checks or using credit cards without permission or under false pretenses
- Changing names on insurances, wills, financial accounts or property titles
- Charging an elder for products or services (such as high-fee loans, investments or insurance products) that are unaffordable or inappropriate for the elder, especially when the elder doesn’t authorize it, or deceit is used to gain authorization
It’s upsetting to say, but there are many unscrupulous businesses that may coerce a senior into signing up for renovations or home repair work that is expensive and un-necessary. Some of these shady businesses may present themselves as working with senior-specific programs, but it’s always essential to do your due diligence and research the real, legitimate state and national programs that offer free and discounted home repairs to elderly seniors.
Healthcare fraud is a specific type of financial abuse that occurs when healthcare providers engage in unscrupulous activity such as billing for services not rendered or prescribing inappropriate treatment for their own financial gain.
5. Elder Neglect
Elder neglect occurs when a caregiver fails to fulfill their obligations to meet an elder’s needs.
Neglect can be either passive – when the caregiver is unaware of needs that they should be aware of – or willful. Willful deprivation occurs when food, assistance, medical care or other necessities are purposely withheld.
Examples of neglect can include failing to provide adequate:
- Food, hydration or nutrition
- Shelter
- Hygiene assistance
- Medication
- Health care when needed
- Activities for social and mental health wellness
6. Elder Abandonment
Abandonment is a severe form of neglect. It occurs when a caregiver has assumed responsibility for care or custody of an elder and then leaves them without arranging appropriate replacement care.
7. Elder Self-Neglect
Elder self-neglect occurs when an elder fails to meet his or her own needs.
Self-neglect may be a result of dementia, depression or other physical or mental health condition that make it hard for them to realize or meet their own needs.
Signs of Elder Abuse: What to Look Out For
Signs of elder abuse can be difficult to discern at times. While a pattern of obvious bruising or injury might be apparent, other signs can be subtle.
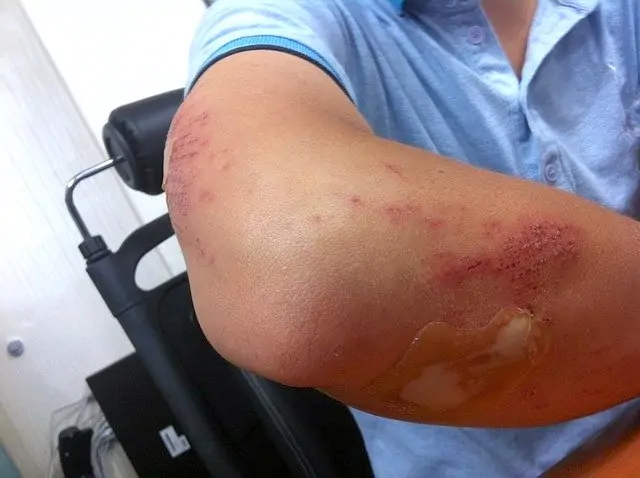
Symptoms of abuse may manifest as vague behavior changes, which might be hard to distinguish from symptoms of dementia or depression. Pay attention to any intuitive feelings that something may be wrong in a senior’s situation.
Some of the more general signs that something is wrong could include:
- Sudden changes in behavior, such as becoming more nervous, jumpy, aggressive or withdrawn
- Losing interest in favorite activities
- Difficulty sleeping
- Unexplained or sudden weight loss
Any of these changes could indicate that an elder is emotionally distraught, which could be a result of physical, emotional or sexual abuse.
It also could mean that some of their needs are being neglected. For example, weight loss could indicate that their nutritional needs are changing and that the change is being overlooked.
Other signs that should raise some red flags to possible abuse could include:
- Increased nervousness around a particular caregiver
- Hostility or frustration in the relationships between an elder and the caregiver
- Threatening, controlling or demeaning behavior from the caregiver towards the elder
- A caregiver who won’t permit the elder to be alone with trusted friends and family members
Signs of Senior Physical Abuse
Aside from the general signs listed above, potential signs of physical abuse could include unexplained bruising or injuries.
While some elders do tend to bruise easily, be alert for “suspicious” bruising such as:
- Patterns of bruises resembling fingertips
- Symmetrical patterns of bruising on both sides of the body
- Bruises, cuts or abrasions on wrists or ankles
- Unexplained bruising or bleeding from the lips, cheeks, face or head
- Bruising in odd places, such as the abdomen or underarms
Signs of Elder Sexual Abuse
- Bruising around breasts, buttocks or thighs
- Bruising or tearing around genitals
- Unexplained bleeding from anus or vagina
- Ripped or bloody underclothes
- Unexplained venereal disease or infections
- The elder stating or hinting that abuse, including unwanted advances, has occurred
- Odd interactions between the elder and possible abuser (such as the elder appearing tense or uncomfortable with another person’s touch, or another resident in a memory care community seeming somehow too close and intimate)
Signs of Senior Financial Abuse
- Unexpected eviction notices or utility shut off
- Unexpected bills
- Unpaid bills, especially if someone is supposed to be helping manage finances
- Unnecessary services or subscriptions
- Cash or items of value are missing
- Suspicious changes to wills, property titles or other legal documents
- Suspicious bank withdrawals (such as unexplained large sums, or withdrawals from a location that the senior couldn’t have accessed)
- Duplicate billings for medical services, or billings for services not rendered
Signs of Senior Neglect
Red flags that neglect, or self-neglect, may be occuring include:
- Unkempt appearance, such as messy hair and clothing
- Poor body odor
- Home appears unclean or unsafe
- Dressed inappropriately for the weather
- Not using or wearing hearing aids, braces, or other medical devices as they should
- Evidence of medications being taken inappropriately (such as too many pills remaining when it’s time to refill)
- Bedsores or signs of inadequate care (wearing soiled incontinence products, bandages not being changed as required)
Changes in sleeping, eating and behavior can be general signs of abuse, but they can also be signs of other conditions, such as depression. If left untreated, these changes can lead to worsening health, lower quality of life and even an earlier death.
If the caregiver doesn’t notice these changes, it could qualify as neglect, because failure to treat the medical condition results in harm upon the elder.
While the caregiver may not intend to neglect the elder, it is important that they are either able to recognize and meet their needs, or to involve someone else who is. Geriatric care managers, home care agencies or other services can help support the elder and their caregivers, and recognize these changing needs.
Not all of these signs necessarily mean that abuse is taking place. However, they should be taken as red flags and may warrant further investigation, especially if there are multiple signs present. If something just doesn’t seem quite right in the situation, do not ignore it.
What to do When Signs of Elder Abuse are Noticed
It’s essential to always be on the lookout for abuse — especially considering that, according to elderly abuse statistics, senior abuse has increased even more dramatically since the COVID-19 pandemic.
Many times, elders won’t be willing or able to discuss abuse, but if they do express feeling concerned or taken advantage of be sure to listen. Speak to them privately, in a safe and comfortable environment.
Even if an elder has dementia, and may not always be accurate in their details, it is important to listen and investigate their concerns.
Depending on the situation, it may be appropriate to first talk directly to the elder or another involved person – such as a family member, paid caregiver or facility administrator – about your observations or concerns.
You can also always report your observations to Adult Protective Services. These professionals are able to take a closer look at the situation and have resources to assist the elder.
How to Report Elder Abuse
If an elder is in life threatening danger, call 911.
Any other suspected mistreatment of an elder should be reported to Adult Protective Services.
Calls can be made anonymously and callers do not need to know with certainty that abuse is occuring. Callers simply report their concern, and a professional will be assigned to investigate the situation.
If the senior’s safety or well-being is at risk, Adult Protective Services will initiate the appropriate interventions.
Elder Abuse Frequently Asked Questions
Who is most likely to abuse the elderly?
Statistically, family members are the most likely to commit abuse, accounting for 60% of cases. Adult children and spouses are by far the most common.
Long term care staff also account for a growing number of cases as more elders reside in care homes such as skilled nursing homes and assisted living communities.
Why does elder abuse go undetected so often?
Because elder abuse is so often committed by people they know and trust, elderly victims of abuse can be hesitant to report them.
They may not want their loved one to get in trouble. They may feel embarrassed or ashamed, or they might excuse the abusive behavior in their own mind.
Since the abuser often is a key caretaker of the elder, they may fear what will happen to them if they do report it. Will the abuse get worse; will they be put in an institution or left all alone?
Many elders are unable to report abuse due to memory or communication impairments, or for other reasons.
Some elders may not even realize what has happened at all, such as in the case of financial exploitation. They may suddenly find themselves without funds, facing unpaid bills or an eviction notice, and not know how to handle the situation.
Elder Abuse: A Hidden Epidemic
Elder abuse has been called a hidden epidemic that impacts the health and wellbeing of six million elders annually in the United States alone.
By being aware of the problem, the potential signs of abuse and the steps to take when these signs are noticed, we can make a big impact on this epidemic as a whole. We can make an even bigger impact on the health and well being of each individual elder for whom we speak up.

Have you noticed any signs of elder abuse in a senior you know? What did you do? We’d love to hear your story in the comments below.





I am being charged $11,486 for a simple basic walk – in shower I was made to believe would cost between $800 and $1,000.
Hi Lawrence, I’m afraid we can’t offer legal advice, but it might be worth reaching out to a lawyer who specialized in elder abuse. Good luck! I’d also suggest reaching out to local senior services if you need help finding good legal advice.
I understand there is a form of elder abuse where confidence is undermined and victims are confinced they are losing abillity to cope with day to day responsibilities, this results in being verballed into positions where they are confinced they have agreed to certain actions which they cannot remember having given their permission to.
What is needed is in associations that the abuser connects with landscapers in management of asso to encourage all events to bring your own boos to break down inhabitions you document what they’ve said under drinking influence to set them up through terrorizing their units using maintenance and landscaper and Mgmt free up units for commissions. Then a final blow is to encourage poor roofing to not put paper under roofing tile to cause major evacuations with soaked furniture. I’ve witnessed this to document Association protection for criminal activity
I’m 86 yrs old and need help in removing a girl age 25yrs old from my home.She never paid rent but now I dont want it.She called police on me saying I was putting her out .He told me I could not go in her room .I’m worried cause I know she is on drugs please help me .Remove her
The only thing I can think of is does she have mail at your address, did she have any of her furniture there? If there is a yes to any of these things you might have to file an eviction notice through the court or another thing is get a restraining order of protection again her.
Good luck to you !
I live in an apartment setting whereby 3 apartments share a laundry facility. We are to clean up after ourselves. I am going on my 10th year of living here. The laundry room is always left a mess when I need to use it. Recently, I spend 5-8 hours sanitizing because cat urine is so strong in the appliances I cannot wash my clothes until the smell is gone. I have used a $ 27-gallon jug of sanitizer in a month. I have talked to management over and over. Some of these renters washed all hours of the night and my hollow core kitchen door leads right to the laundry room. I have been threatened by one of the tenants, who thankfully no longer lives here. I used to lock the door when I was using it because, with only one appliance each, nobody else needs to be in there. I was told, “unlock that door and you’re scared of everytthing”. by the manager I had neighbors so out of control on the other side, that I had to move my bed to the living room so I could sleep. I called the cops and then was threatened by the cop that I was harassing her. I have audio, video, and photos to back up my claims. This is my 40th year of teaching and I’ll be retired and getting out of this building but it could be another year of hell. It has impacted my well-being.Nobody should have to live this way.
I live in a mobile home park where there is a grass cutter within the premises, I decided to change grass cutters cause I wasn’t satisfied with his work. Now he is harrassing and bullying me. What can I do?
My neighbor has taken me to court 70 +/- times. I am 68 she lies in court and lies to the police and has sent me to jail twice. First time my cats almost died from lack of food as I have no one here to care for me or them. I have one more court date where she and her husband were on my property. A judge told her three times to stay of my property. I have a fence 3 ft from my property line to avoid damaging the water line The judge is aware of this. She has taken me to court so many times and lost all cases. All this has cost me 27K which keeps me from getting my teeth fixed or removed.
I am married to a friend of mine who is now in his 70s. He is fiercely stubborn and resists advice of any kind. He will not do anything to help himself (hearing aids, teeth, glasses) and says he’s fine. As friends we have always argued and I’ve yelled at him a lot over 40 years; he’s difficult and frustrating. I am now reading our normal historical relationship pattern may now get me into trouble. Do I divorce and leave to save myself as there is no reasoning with this man and he won’t accept advice. He’s not impaired yet at all but I am concerned about the future. I can’t be responsible because he doesn’t want anyone in his business
That’s a really tough situation Roberta. No easy answer for sure.
I was told that I had several small strokes in November 2019. I have lost about 4 to 5 months of memory after I had the strokes. My cousin was put in charge of my medical, this was decided without my knowledge. My cousin moved into my home without my knowledge to take care of my dog. My cousin in turn got a puppy, my daughter told me that we had made a agreement that my cousin and I would go and pick out a dog together when I got out of rehab. When Iwas able to get around and get on my laptop I found that my cousin had changed all my passwords to akk my online accounts including my bank and Social Security. It took me a long time to get all my passwords changed. When I finally got into my bank account I discovered that my cousin had started writing checks to theirselves two days after I went into the hospital. My cousin used my checking account, food stamp card and my debit card for everything. I recently found out that I was prescribed a small dose of oxycodone but I never got it to my knowledge, my cousin has stolen oxycodone from me before and I had to lock my medicines up so my cousin couldn’t have access to it. My daughter ndoesn’t want to be involved if a file a claim of elder abuse against my cousin but I think she should have to pay for what she has stolen from me and the money she took which is around $6000.
I’m so sorry Katherine, that sounds really terrible! I hope you can find someone to help you locally.
I’m sorry too. And I am sorry you are getting such weak replies from an agency that is supposed to be helping others. These people are appealing to you, Megan and others here, for some kind of help, advice, etc. The answers you provide are not of any significant help.
Lana, I am no type of agency. I am an individual who runs this site to offer information where I can to those in need. Anyone experiencing elder abuse needs to contact their local agencies in their individual areas.
Who can i speak to regarding elder abuse of emotional & financial nature
My late husbands 91 year old aunt is in rehab center for past 4-5 weeks her niece inherited family home sold it & has not supported aunt i past 4-5 years. She has POW & decided after her uncle died that she was not going to help her aunt financially although uncle was assisting her before he passed away. Niece has refused to talk to aunt or have any contact with her. Aunt has been dependent on friends for her financial help, Since the home was the family home she expected to inherit something & niece took unccle to her friend a lawyer to make up the will & she recently told my husband before he passed that the lawyer told her to not give aunt any money because she’ll only ask for more All aunt talks about is getting in touch with this niece
I’m 90. I was tricked out of $331 which I wouldn’t have paid except for lies and threats made against me. I filed suit to regain the money. Judge promised a trial date, in writing. Days before the trial, judge changed mind, dismissed suit, on illogical grounds that I could have responded to, if the promised trial had been held. Since then, judge has made the false claim that I had groveled for reconsideration (I hadn’t) and implied that I had alleged some sort of conspiracy (I hadn’t). Unable to afford an attorney, I’ve now faced several years of negative emotional input due to having no access to rights I believed were inherent, and the prospect of the judge’s caprice making public records reflect an unflattering image of me. I feel the judge was abusive. Is this valid?
Burton, I am just a common, concerned citizen, not in authority of anything, but I just wanted to say how sorry I am that things like this are happening, and that they happened to you. It is just awful and disgusting that people do not value older ones, but instead see them as someone they can (almost legally) take advantage of and kick around with impunity. You’ve lived a long life and shouldn’t be facing so much hardship in your golden years. Please know that I, and I’m sure there are others here, who would assure you that you are worthwhile, and do not deserve this abuse. I wonder if Legal Aid could offer you free legal advice and help? It might be worth a try to see what they can do for you. Here’s hoping that you are able to get some relief and resolution to this terrible situation.
Lana,
Your article was very informative! While you obviously care about the issues at hand, your invitation to leave stories results only in pleas for help that you cannot provide. These people who are leaving the experiences are mentally in a different place than you All you can give is words of sympathy and a “good luck.” Instead of unintentionally giving false hopes to your readers, do your due diligence and provide a real list of resources for help…give them real hope. Though it is affirming that people are reading your article by leaving their experiences, let these people spend their energies in a productive, problem solving way. They gain nothing by leaving you their experiences.
Hi Dawn – first of all, I think you are referring to Laura! Secondly, this article is about different forms of elder abuse and how to recognize them. Not about how to resolve these issues. Each situation is nuanced and required individuals to work with their state and regional resources. I also disagree — sharing eachother’s experiences helps those who are suffering feel less alone. I’m sorry you can’t see the value in this piece, but I assure you it’s helped many people.